History of Neurology at the UW
08/21/12 | 52m 57s | Rating: TV-G
Andrew Waclawik, a professor in the Department of Neurology at UW-Madison, introduces clinical neurology by way of its historical background. Waclawik reviews the origins of the new clinical specialty in the 19th century in major European medical centers, and presents the history of neurology at the University of Wisconsin.
Copy and Paste the Following Code to Embed this Video:
History of Neurology at the UW
cc >> Good evening. Thank you for watching Wednesday Nite at the Lab. I'm Cassie Immel from here at the Biotechnology Center. This evening we'll be hearing from Dr. Andrew Waclawik. He is a Professor of Neurology here at the UW in the School of Medicine and Public Health. He graduated from Warsaw Medical Academy in 1982. He did his residency in neurology at the UW Hospital and Clinics in Madison and subsequently completed his fellowship in neuromuscular diseases at the Mayo Clinic in Rochester, Minnesota. In 1993 he joined the UW Neurology Department faculty where his clinical and research interests have been focused on neuromuscular diseases and muscle and nerve pathology. Dr. Waclawik is a fellow of the American Academy of Neurology and the American Association of Neuromuscular and Electrodiagnostic Medicine. So, without further ado, here's Dr. Waclawik.
APPLAUSE
>> Can you hear me? Well, thank you very much for the invitation. My name is Andy Waclawik. I'm a neurologist on faculty at the Department of Neurology. I'd like to tell you briefly how this lecture came about. Approximately two years ago, many physicians moved offices from the UW Hospital to this new building called Centennial Building, UWMF Centennial Building, to recognize the hundredth anniversary of our medical school which was quite recently. So, about this time when we were kind of moving to a new place, we were hanging the group photographs of old and the more recent faculty, we decided maybe it's a good time for some type of a reunion. And some of us, and especially our chair Dr. Tom Sutula, started making some phone calls to some old, retired faculty, some of the past residents, fellows, and students, and we celebrated this recently in June. So I was asked to give some presentation, maybe because of my interest in the history of neurology and how neurology actually came to Wisconsin, how it was practiced, and who are the most influential people who helped to build the Department of Neurology and lead it to the current success. So, eventually, I was contacted by UW by Tom Zinnen to maybe give this presentation to a different audience. So I tried to simplify some of these slides and simplify this message, but actually the core information is very similar to what I presented in June. So, I'm not sure if everybody knows exactly what neurologists do, so I went for the ultimate source of information to Wikipedia trying to find out what I actually do.
LAUGHTER
I found out that neurology is a medical specialty dealing with disorders of the nervous system. To be specific, it deals with diagnosis and treatment of all categories of disease involving the central, peripheral, and autonomic nervous system, including their coverings, for instance meninges around your brain, we treat patients with meningitis, blood vessels, and all tissue such as muscle. This is actually my specialty. I see patients with so-called neuromuscle conditions affecting peripheral nerve, neuromuscular junction, and muscle. The corresponding surgical specialty is neurosurgery. And historically, neurosurgery had a lot to do with neurology, and some of the panels of neurosurgery, including a famous French neurologist, were eventually encouraged to go in the direction of neurosurgery. So, let's continue. A neurologist is a physician specializing in neurology and trying to investigate, diagnosis, and treat neurological disorders. Neurologists may also be involved in clinical research and clinical trials as well as basic research and translation research. Neurology, being a branch of medicine, differs from neuroscience which is the scientific study of the nervous system in all its aspects. I want to add to this that, historically, we are very much linked to psychiatry, and many neurologists actually, at least at the end of the 19th century and also the 20th century, were also double boarders. They were specializing in both neurology and neuropsychiatry. They practice in both disciplines. This is my father who is now 91 years old and practiced neurology for 50 years and also practiced as a psychiatrist. So, you appreciate the history of neurology, immediately you enter our department. We're on the seventh floor of the Centennial Building. You push number seven and you leave the elevator, immediately you see this display. The center of this display is this percussion hammer. Now, percussion hammers come in different shapes and sizes. They have different names. Many of them were named after the neurologist who used them or designed them. For instance, this is a Trimmer Hammer. This would be --. This would be modified by --. This is probably a modified Queen Square hammer. But this hammer is not any percussion hammer. This was used by one of the greatest, if not the greatest, clinical neurologists ever. Famous Polish-French neurologist Dr. Joseph Babinski. He was the master of clinical bedside examination techniques. And much of the examination that we do at bedside was probably finalized by the late 19th century by great French, British, and German, and some other neurologists, and what we do nowadays is very similar to what, actually, Dr. Babinski was doing over a hundred years ago. So, when you look at this, that's how he looked when he was a resident with famous --. When you remember Babinski, you might know that his name was immortalized by a famous Babinski sign. There is probably no other sign in neurology, and probably the whole medicine, that is more recognized than Babinski's sign. You talk to a student in the US, you talk to a student in England, Germany, India, Australia, they will know what Babinski's sign is. And probably some of you who might have seen neurologists were intrigued. What, actually, they are looking for, they are stretching my foot and they are trying to find out what side of the brain is sick. So, this is a sign which was described by Babinski in a very short report in 1896 when he discovered that actually the natural plantar, which is a response that is typically flexor, the toes go down when you stimulate the foot, the toe may go up in certain conditions affecting so-called pyramidal or corticospinal tract which is the major motor pathway connecting the brain with the spinal cord. So, Dr. Babinski made major contributions. We probably remember the -- but he made contributions in semiology of the corticospinal tract, diseases, cerebellar conditions. However, he was also a most respected and looked after to get some additional training. And many neurologists from other countries, including American neurologists, went to Babinski in Paris to train with him. One of the most famous ones was Dr. Charles Charter from St. Louis, who trained with Babinski and made a few trips to Paris. He was also a friend of Henri Babinski, Babinski's brother, who was a famous cook and wrote a book on cooking. So when you look at this percussion hammer, you can immediately see this name. Dr. Babinski, from Dr. Babinski in Paris to Dr. Charter in St. Louis. So, Dr. Charter eventually gave the hammer to Dr. --, his favorite student who eventually gave this to Dr. Reese, who was one of the first chairmen of our department. He actually gave this to Dr. Forster, and he gave this to Dr. Schutta, and currently it's owned by Dr. Sutula, our current chairman. So, when we want to talk about the beginnings of neurology, before I go to the origins of neurology in our state, I'd like to give you a very brief overview of how neurology evolved. Neurology is a new specialty evolved gradually in the course of the 19th century, especially in the second part of the 19th century. And three major European centers, especially the one in France, in Paris, Salpetriere with Jean-Martin Charcot, the English center around the Queen Square with many influential British neurologists, especially Hughlings Jackson, and in Germany. Obviously, there are many influential neurologists, and I cannot review in detail how many brilliant neuroscientists contributed to the modern specialty, including Russians, Romanians, Polish, and Italians. So that's the mecca of neurology, and anybody who wants to be a neurologist has to go at least once to Paris to see where it all started at the Salpetriere. Now it's called Pitie-Salpetriere because the small hospital where Babinski practiced was now attached with his name. So, just to give you some timeline, this is Jean-Martin Charcot, who truly deserves to be named as the father of modern neurology, and the date 1888 is probably now recognized as the beginning of neurology. Obviously British strongly dispute this, but that's not the first time they challenge the French. This is Dr. Duchenne, Duchenne de Boulogne, who someone influenced also Dr. Charcot and collaborated with him. You probably recognize his name from Duchenne dystrophy. If you watch the September telethon, Jerry Lewis, MDA Telethon, that's the name attached to this. And here's Dr. Babinski, who was a student, probably one of the most celebrated students, of Dr. Jean-Martin Charcot. So, this is probably one of the most famous paintings in a clinic in Madison called Clinical Lesson at Salpetriere by Andre Brouillet. You see the famous Dr. Charcot. This is Dr. Babinski holding this patient who probably has some hysterical conversion reaction. And here are the famous celebrated students. They all became brilliantly celebrated and internationally recognized neurologists. So, this is the building of the National Hospital for Diseases of the Nervous System including Paralysis and Epilepsy which was founded in 1859. This was then renamed this several times, but British believe that this date is the beginning of modern neurology. I just want to want to recognize two names of John Hughlings Jackson, who did some work on the semiology of epilepsy including focal epilepsy, William Gowers, which is close to my specialty from many descriptions including Gowers' sign. This is probably a group of the most influential German neurologists, Wilhelm Heinrich Erb, who practiced in Heidelberg, --, and Hermann Oppenheim practiced at Charite in Berlin. Now, this wouldn't be possible if not for the contributions of all brilliant neuroscientists who gave us the foundation to modern clinical specialty. I will mention the one name which is somehow dear to my heart because I'm also a physiologist, Emil du Bois-Reymond who discovered so-called negative Schwankung which is now known as action potential. He was not only a brilliant neuroscientist, neurophysiology, he was a great philosopher, a great speaker. He gave many influential and frequently transcribed lectures on different topics and politics, philosophy, sciences. Together with Helmholtz and Carl Ludwig and Brucke, they founded the famous Berlin German School of Physiology, modern school of physiology, which strongly rejected the concept of -- that humans and animals have some special forces which are not present in non-living organisms. He strongly rejected this. He was convinced in reductionist and he believed that humans and animals should be studied with the same principles of physics and chemistry as non-living objects. So, back to Charcot, surely deserves to be remembered as the father of neurology, and he invented so-called clinical anatomic method. It might sound so simple, but actually, what they were doing, patients at Salpetriere, which was an asylum for very sick and mental patients, once they were admitted, they would stay until they would die, most of them, sometimes for decades. So he introduced this system of very detailed meticulous record-keeping with descriptions what they observed, what kind of symptoms patients had. Frequently this was accompanied by these drawings in patients' records. Dr. Charcot himself was a talented artist and many of his students were encouraged to draw paintings or to draw pictures of patients, especially with some special clinical signs. So then if a patient passed away, if they died, they would have an autopsy, frequently done by neurologists or some pathologists, and they would look what was wrong, what was wrong in the brain, what happened to the spinal cord. They would dissect peripheral nerves. They would dissect muscle and try to correlate the very much detailed longitudinal observations with abnormalities of the brain and spine. That's how, actually, many conditions were discovered, including multiple sclerosis or amyotrophic lateral sclerosis, known as Lou Gehrig disease in the US, known as Charcot disease in France, and the progress in understanding of Parkinson's disease, different tremors and so on and so on. So this was actually quite new at that time. This was combined with continuing progress in bedside clinical examination techniques. I mentioned Charcot, but there were many other neurologists from different countries who improved the bedside examination techniques. So, sometime at the end of the 19th century, just around World War I, the modern clinical examination was well organized. The way we examine patients is we check mental status, speech, we check cranial nerves, we check motor system, muscle bulk, muscle tone, strength, reflexes, sensation. This was well standardized already over a hundred years ago. And nothing's changed much. Nothing has changed much so far. If anything, the art of clinical examination has declined, but that's not unique for neurology. I think the same may be said by other specialties. The technology is now overwhelming and the students probably are not as good as they used to be a generation or two ago. So, neurologists were somehow moderates where there was something special about the brain, and people who would go to neurology were very much thought to be the smart people. And anything new was discovered in technology, engineering, in sciences, was immediately translated to using clinical science. I will give you some example. For instance, the art of photography was introduced by medicine by Duchenne, the one who collaborated with Charcot. So when the wet plates came and the exposure times were shorter, he immediately recognized this is a very powerful tool for clinical documentation. He can now take a picture of a patient instead of drawing and share the picture with you colleagues and publish this. So, there was no more need for drawing this picture. There are some original pictures done by Charcot of patients with muscle dystrophy and findings from a muscle biopsy. So this is a picture of the first published item of photography. At that time they couldn't print photographs, so these would kind of accompany the printed textbook. So this is the first ever in the history of medicine done by neurologists. So, I will not spend much time talking about the specific conditions. This is probably Duchenne dystrophy. This is so-called facioscapulohumeral muscular dystrophy and other conditions that some colleagues in audience who are neurologists may recognize. So, just to show you what kind of visuals they were, the French have a lot of talent for engineering. They have this art of so-called bricolage, they all kind of tried to invent something in the garage. So Duchenne actually invented this tissue, this muscle biopsy, and actually, what I use these days is essentially a copy of what he invented over a hundred years ago. Another invention which was immediately incorporated into clinical practice was the invention of cinematography. When the Lumiere brothers had a public presentation at the turn of the century, they traveled, and their associates, to many countries. They went to Bucharest, to Romania, and the famous -- who was one of the students of Charcot, immediately recognized the potential for a neurologist. So he was captivated by this new art of movie making cinematography and published several papers between 1898 and 1902 based on his observations. I hope some of these clips work. So, this is one of the first, if not the first, movie clip made capturing the normal gait of a patient, possibly a young resident, a young physician. The next clip... >> What year was that in? >> These clips that I'm showing you were made between 1898 and 1902. That's when they actually were published. So very, very old. This was actually digitized by American Academy of Neurology. So some Romanian neurologist found this original film. This was digitized eventually. This, actually, you will appreciate quite a lot. This is a picture demonstrating a woman who has hemiparetic gait which is non-organic. At that time, actually, many physicians were very skilled in the art of hypnosis. So look what happens. This woman has the hemiparetic gait. She's dragging her leg. She gets hypnotized. And she has normal gait. So this was immediately recognized as a very powerful clinical tool for neurology and for medicine. Another example, when Michael Faraday published his work on electromagnetism, induction cause came to use. Again, famous Duchenne jumped on this idea that this can be useful for muscle nerve stimulation. At that time, galvanic stimulation was a very low intensity. They couldn't get these muscle nerves stimulated. So he started inventing and improving on these small induction coils and stimulating muscle and nerve. And actually, many French physicians used these induction coils as part of bedside examination. If the extremity was paralyzed but the muscle was still twitching to direct stimulation, it was probably central. If the muscle didn't twitch, this could be peripheral. So there was eventually ongoing progress in different techniques including introduction of x-rays, then actually the major improvement discovered was introduction to lumbar puncture. An examination of the cerebral spinal fluid has given us a window to examination of the nervous system in vivo. So, these clinical improvements were backed up by continuous progress in neurosciences. I will just mention Camillo Golgi and famous Cajal Golgi for his --, Cajal for his many contributions including the neuron doctrine. So, neurology was ready to come to the big stage. But let's go back to Wisconsin. In the middle of the 19th century there was not much of medical practice, of standardized medical practice. We were still a frontier state. There was incredible poverty in this state, malnutrition, infectious diseases, and farming accidents, and the practice of medicine was very poor. Physicians were poorly trained. Many of them didn't have any formal training. The ones that were better trained were possibly foreigners, immigrants, or came from other states. But our founding fathers who drafted the constitution had a vision that we need a big university, strong, public university that should include, eventually, a medical school. Now, we took many years for fruition of this idea. The most important person was Charles Van Hise. Now, in his now famous speech in 1904 with his so-called Wisconsin Idea, he said, "I shall never be content until the beneficent influence of the university reaches every home in this state." What better he can do for the people of Wisconsin than improve the healthcare? So, he relentlessly pushed and pushed, and eventually he was successful in the recruitment of Dr. Charles Bardeen who came from Johns Hopkins. He was a great anatomist who was appointed chair of the Department of Anatomy, who eventually recruited a famous Dr. Erlanger, great physiologist who got Nobel Prize in 1944. And the core faculty was there for physiology, anatomy. They recruited more people eventually. The two-year program was established in 1907. So most of the students who graduated from this two-year program had to go to Chicago or Cincinnati or some schools on the east coast to get a full medical degree. But in 1925, a full four-year MD program was established. Just to give you some sense of history, that's how the Bascom Hill looks nowadays. So the teaching of basic sciences was excellent. It was better by progressive recruitment of more clinical faculty. They built new facilities. This is just to show you so-called student infirmary which was built the same time as Bradley Hospital which was eventually attached to Wisconsin Hospital. So we were ready. But to go to neurology we have to, again, go back in time. Now, this is very old picture showing Wisconsin Hospital for the Insane. This hospital was built in 1860. This was a great building, grandiose building, palatial building. One of the most beautiful in the country. This was built on the northeast shore of Lake Mendota. There's not much left from this original building which was like an asylum for mentally disturbed patients. But if you want to read some more about this, you may want to read this book which was given to me by a friend of mine who works at Mendota. This is about the first intendeds of Mendota Hospital who was a very controversial and disturbed person but is a great source of information about the history of that place. Now, this was renamed in 1935 and later in 1974, and now it's known as Mendota Mental Health Institute. There are many different buildings. Some of them were built before World War II. Some of them are new buildings. It's a great park actually, and you can go there and visit that place. There are many hiking trails, and it's a beautiful place to go and to learn some history. So, this hospital that you see is actually not the original building. This was built in 1922 to accommodate World War I veterans with mental conditions. This building has been now empty for over 20 years. Apparently, it's the most haunted house in Wisconsin.
LAUGHTER
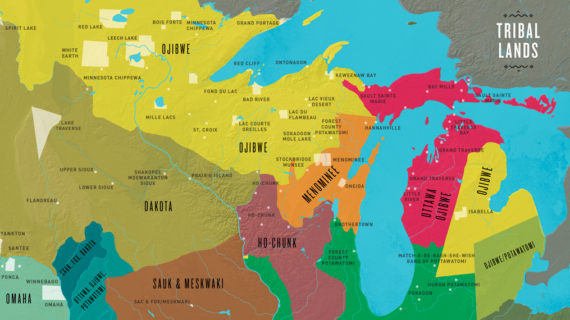
Now, just across the building, if you go there, you will see these beautiful Indian mounds. I'm not an expert in this field but I was told that they are one of the most special and most beautiful mounds you can see not only in the state of Wisconsin. Some time in 1907, the superintendent of Mendota Mental Hospital drafted a plan for a 10-year expansion which would include a research facility and hiring of a neuropathologist who would also be appointed as faculty at the University of Wisconsin. Now, neuropathologists were difficult to find but they were able to recruit Dr. Lorenz who trained in New York City and trained in psychiatry and neuropsychiatry and came to Wisconsin. Now, he was eventually appointed director of the Mendota Hospital, and in 1914, he was appointed the first director of this so-called Wisconsin Psychiatric Institute which was this clinical research facility on the grounds of Mendota. Now, when the new Wisconsin State Hospital was built, he moved the WPI to the main building, and this was the beginning of the so-called neuropsychiatry department. He made many important contributions. Among others, he introduced the -- test which was used to test blood samples and spinal fluid on patients with suspected syphilis. This was a major public issue at that time. He also, because of his interests, established very fruitful collaborations with many scientists on the campus. I will mention his collaboration with Dr. Levenhart who was the head of pharmacology. They developed the use of trypanosomes in the treatment of syphilis, of neurosyphilis. This compound actually was developed by -- Institute for treatment of African sleeping sickness. But they recognized the potential of using this to treat syphilis. So there are many traces of Dr. Lorenz in Mendota. If you go there, you will see many signs or even a building named after him. That's how the hospital looked in 1924 when he moved the WPI, Wisconsin Psychiatric Institute, and this became the psychiatry department. Just to give you some perspective of time, this is how it looks now. And this is actually a photograph that I like showing you how we looked at the future showing the Discovery Center, but we always look to the past as well in Wisconsin. So, probably the biggest accomplishment of Dr. Lorenz was hiring Dr. Hans Reese. Now, I may not have enough time to tell you his life story, which is a fascinating story, but one of the guests today, Erika Janik, I should probably say Janik because it's a Polish name, who is a most talented writer wrote a big story which will be published in the Wisconsin Alumni Magazine probably around September or October. She's also married to my distinct colleague Dr. Matt Jensen. They collaborate on many neuroscience projects. Let me mention a few things about him. He was born in Germany. He graduated in 1916 from medical school in Kiel, Germany. He served in the German navy and was decorated for his service in the German navy. Eventually, sometime in life he recognized that the has a lot of intelligence in sports. And there's no bigger sport in Germany than football, soccer. Soccer is bigger than life. So he was a prodigy in sports. You can see him on this picture of the team, Holstein. And eventually he was so good that he was selected to represent Germany during the Olympic games in Stockholm. You can see him right here. This is before the match with Austria. They won two to one. So, this is just as we finished watching one Olympics, I want to give you one example of another great neurologist who actually was a superb athlete, famous sir, he was knighted, Roger Bannister. This is the person who, for the first time, ran a mile under four minutes. He's the man who said, "The man who can drive himself further once the effort gets painful, is the man who will win." Now, he eventually trained in neurology at Queen Square in London, together with Dr. Schutta, who was our chairman. They became friends and we always heard stories about Dr. Bannister when I was training in neurology at UW. But he, himself, was an established neuroscientist, neurologist, especially in the research on autonomic nervous system and became director of the National Hospital for Nervous System Disease in London. Now, when we did some research on Hans Reese in the UW archives, we found his notebooks, and being a neurologist, I immediately appreciated the beauty and the detail of his notes from his neuroanatomy lectures. You can see the pictures of the brain stem, some sensory organs, the inner ear, but this one is quite spectacular. You can see a picture of the nervous system and some of the pathways connecting the brain with the brain stem. Here he writes -- consequence of lesions. Now you can actually take this picture and print this in any modern textbook. I guess only Germans can do this so well probably.
LAUGHTER
So, he published papers on all kinds of conditions but the major work he did in the '20s was in treatment of neurosyphilis. This is something which may surprise you, disturb you, and shock you, how they treated neurosyphilis at that time. Those of you who may have some background in microbiology may know something that there is primary, secondary, and tertiary syphilis when this effects nervous system, brain, and spinal cord. This was a major public issue. Up to 15% to 20% of patients admitted to psychiatric hospitals suffered from neurosyphilis at that time. So physicians were desperate to do something. Now, this was the '20s. Syphilis was prevalent in Paris, London, and Berlin. It was affecting rich and poor, famous kings and politicians. So it was a disaster to see those people dying with this terrible dementia and psychiatric disturbances and frequently with other neurological deficits. On the other hand, one has to be careful because we frequently hear stories about famous people dying from neurosyphilis. For instance, they always say that Friedrich Nietzsche had neurosyphilis, although there is not much solid data to support this. This is only by associating some of his lifestyles with the psychiatric disturbances that he exhibited later in life. There was no autopsy, as much as I know. There was no serology at that time. Some people believe that, actually, he suffered from a mini stroke or something that we we refer to as frontal temporal dementia. But this is another demonstration of what neurosyphilis was doing to people and still does in some places. And sometimes is may affect the spinal cord and cause --. When it affects especially the pathways for sensations for perceptions, these patients have terrible gait ataxia. This is, again, a movie clip made by the Med School, published between 1898 and 1902 showing this patient with so-called locomotor ataxia. Just watch how this manifests. So, these patients had to be supported by the physicians or the nurses, otherwise they would fall. So it was a terrible disease. So, the idea about treating of patients with, infecting them with malaria was not, obviously, invented by Hans Reese. The German physician, actually Austrian physician, Julius Wagner-Jauregg got a Nobel Prize for this in 1927. He actually invented the concept of pyrotherapy. He observed that if a patient with psychiatric illness has a high fever, they may transiently improve. They may get better. So, what a better way to induce fever than to infect people with malaria.
LAUGHTER
And this was common practice not only in Europe but in other countries as well. So, also people are shocked that Dr. Reese was using a derivative or arsenic. But, actually, Paul Ehrlich also got a Nobel Prize in immunology. He invented, actually, the preparation 606, known as Salvarsan, for the treatment of syphilis. And this was used in 1940s to treat syphilis until penicillin came to practice. So, he actually reported on probably like 64 patients who were treated with malaria infection, and they, according to him, most of them improved. I just to read something for you because some of you do clinical research. Something in the medical which was published in the journal when he reported this. So at that time there was a lot of anxiety that infecting people with malaria because of mosquitoes in Lake Mendota might spread to the population. So he wanted to prove that this is not a risk. And here is what he writes. The occurrence of -- mosquitoes in the Wisconsin lake region necessitated studies of possible mosquito transmission to the community. So that's what he did, he says. In a screened room were placed three malaria positive patients who had chills and temperature from whom we infected new patients successfully. I placed in the same room, two new patients, a new patient with syphilis, leaving the windows open so that many mosquitoes entered and they were trapped. Then the windows and the doors were kept closed. All five patients had many mosquito stings. The two new patients did not develop any infections, none was found in the blood. So, that may be quite shocking to anybody who does research these days. But you have to remember, this was the '20s and there were different standards for clinical research. So, Dr. Hans Reese, again, another personality bigger than life. He was a well respected and well known in Dane County. He traveled a lot. He was frequently visiting Japan where he taught and consulted patients. He traveled to Egypt and other countries and, eventually, was recognized for his service and promotion of good relations between Germany and the United States. I should not mention about his other involvements during World War II when he helped collect intelligence. But this will be covered in this excellent article that you will read soon. I was just passing by Shorewood Hills and I was passing by this sign. So apparently they owned a small piece of land in Shorewood which they donated later as a nature preserve. So, another interesting personality that helped to build our department was Dr. William Bleckwenn. He also came from the east coast like Dr. Lorenz, and he came, actually, to do undergraduate studies. At that time, UW had a strong reputation and many east coast students were coming to do some undergraduate work. Because there was no medical school, he went back to New York and then came back to train at Wisconsin Psychiatric Institute with Dr. Lorenz and Dr. Reese. He was also a talented athlete as Dr. Reese. Now, again, he made many contributions but most famous is his introduction of sodium amytal in psychiatric evaluations. He observed that some patients, especially patients with schizophrenia who may suffer from so-called catatonia when they become stupors and mute and have this form of motor paralysis which we frequently refer to as catatonia with unusual postures. If you inject sodium amytal, they may, for a brief period of time, improve. They may converse. They may engage in some interactions. So this was eventually known as medical -- or medical synthesis. And this amytal induced lucid interval became a proof positive test for diagnosis of catatonia. Now, this was later viewed as beginning of modern psychopharmacology. I don't have to tell you that this was immediately recognized as a potential useful tool for some nasty things. So, this was used for interrogation of prisoners initially by gestapo, by Nazis. It was used by KGB. Eventually it was used by CIA. It took quite a few years to define this as a form of torture, and these confessions obtained with sodium amytal injections, and some similar medications also used as so-called truth serum, were not admissible in courts. We also use now this so-called water test when we inject sodium amytal into the carotid artery when we try to determine the language and memory preference in patients who are prepared for epilepsy surgery. So, in 1958 our department was split. This was something with Dean Bowers. He decided that neurology should go the separate way, and psychiatry with Dr. -- was established also as a separate department. So that's our picture how the core of the faculty looked in 1958. Another great neurologist with international fame was Dr. Francis Forster. He was a professor of neurology at Georgetown and was recruited to lead the department in 1958. Now, at that time there was not enough space at the old Wisconsin Hospital, and actually, neurology was moved to a different building that you can probably still see. This is a building next to east high school. But at that time it was referred to as Wisconsin Neurological and Habitation Hospital. Now, Dr. Forster made many contributions in the field of epilepsy. He wrote a book about so-called reflex epilepsy. This is a form of seizures which may be induced by certain unusual stimuli, like listening to some piece of music or some visual stimuli or some tactile stimuli. But he was an older neurologist and was also very much talented at --. He founded, co-founded the American Academy of Neurology. Some of you might have heard about the importance of Dr. Forster testifying in the famous Jack Ruby trial. At that time, the defense for Jack Ruby had this idea that they wanted to sell to the jury that he suffered from some unusual form of epilepsy at that time referred to as so-called psychomotor variant. When patients may have some alteration of consciousness or loss of consciousness with amnesia, lack of memory, without convulsions. So, Dr. Forster was asked to review the electroencephalography, brain wave test, examine the patient, review the circumstances, and provided a very powerful testimony against this, that Jack Ruby did not suffer from epilepsy. This apparently helped with successful conviction. One person I want to mention, also, who was not in the position of chairperson but was also very instrumental in our medical school and our department was Dr. Eichman. Dr. Eichman was elected dean of the medical school in 1965 when he was only 39. At that time, some of the old senior faculty may remember so-called Bowers affair. The Dean Bowers was very confrontational and an abrasive person, apparently, and antagonized much of the faculty. Eventually, he tried to replace the chair of surgery and this went on for a few years. As you know, surgeons have a strong ego, strong personalities, and it's very difficult to charge a surgeon, especially if the faculty supported him. So eventually, he was removed. This was a terrible time for the University of Wisconsin. This was in the middle of the Vietnam War. The campus was very much combustible. There were riots and they elected him to somehow study the process of reconciliation. He had a very much gentler, charming demeanor and found ways to connect departments and improve the relationships. He was also very strongly supported by students. He actually started a Student Health Services and was director of the Student Health Services at the campus. Now, the major contribution of Dr. Eichman was that he pushed and pushed to build a new clinical science center, and he used the same concept as Professor Van Hise. We need more physicians. The population of Wisconsin grew. We need more doctors. We need more primary care physicians. We don't have good facilities. So that's how this was presented, and, eventually, in 1973, there was a groundbreaking of the new facility. You can see --. This is Dr. Eichman. This is Dr. Middleton after whom the VA Medical Center was later named. And that's how we look nowadays. We had quite a progress. So this is the UW Hospital and the clinics. Our centennial building is right here. That's the Children's Hospital. This is VA. So, I would mention in the closing slides a few other persons who are very much important to our department. Dr. Ray Chun, who was interim chair in 1978 to 1980. He was an internationally famous pediatric neurologist. He was also director of the Waisman Center which you can see in the background. And this collaboration has been very fruitful over many decades, especially for evaluation of patients, children with mental and developmental disabilities. Now, it is interesting how people are remembered. He published many, many, many influential papers and was recognized internationally, but
people remember him from this
the Chun Gun. I used Chun gun when I was a student in the '70s in Poland. I had no idea what this Chun had to do. I thought gun was a gun, but who was this Chun? So, at that time, we had no CAT scan, we had no MRIs, the ultrasounds were very much simplistic. People used the art of transillumination to evaluate children with hydrocephalus. Dr. Chun was not the first to introduce this practice, but, actually, he approached engineers at UW and some physicists to design this instrument, which was a very powerful light bulb, 150 watts, in combination with lenses and filters and some veins to dissipate heat. And this gave this very condensed beam of light and helped to standardize the examination. He was one of the best physicians that you can imagine. He had a special talent. It's very difficult to be a neurologist but especially a pediatric neurologist. You don't only treat the patient, the child, you treat the parents and grandparents. So, his connection was unbelievable. He would enter the room and would light up everybody. He taught us so much respect and humility how we examine these unfortunate young individuals. He said, if the child falls to the floor, you get on your knees, you go to the floor. If the mother cries, you cry with the mother. So, an unbelievable person. I will mention, also, that he was very influential in Dane County, and he was the founding father of the Greater Madison Tennis Association. And those of you who play tennis and remember the '80s, people used to say the greatest doubles team was John McEnroe and anybody. We used to say it was Dr. Chun and anybody.
LAUGHTER
people remember him from this
His tennis was magical. A combination of spin volleys was unparalleled. And it was a great privilege to play and practice with him. In 1980, Dr. Schutta was elected chairman, appointed chairman, and many probably still remember him. He made major contributions in electron microscopy and ultra structure of the central and peripheral nervous system. The faculty grew exponentially and many new sections were added in the '80s. He'll be remembered as the ultimate clinician. He grew up in Poland, but as a young person, when he was 17, he had to escape when Soviet troops were invading the city and did his undergraduate work in Germany. Then he moved to Australia, got his MD degree in Sydney, Australia, then he went back to Queen Square and trained in London with the best British neurologists. Now, his love was clinical neurology. He would see all these resident students during morning rounds in the library every single day. At 8 o'clock we had to present all new cases to him. He would comment, he would analyze, and always provide the historical background. He spoke several languages and read fluently from many sources. So you can see the famous Babinski hammer, which I introduced to you, is right here. This is the Queen Square hammer. This is the original Queen Square hammer. Actually, the American version uses plastic. The British use original bamboo sticks. He had a steady supply of these bamboo sticks one of the residents from Singapore brought for him. You would see this sticking out from his white coat. He had to wear a special --. He was very compulsive about this. When it broke, he would replace it with a new one. And this one was donated to him as a gift by graduating residents for special cases.
LAUGHTER
people remember him from this
So, we had our own here at UW. We had this fantastic clinical teaching every day with our mentors, especially with Dr. Schutta who was my mentor. So he helped us to write papers, write grants, and some of you may remember his wife, who was very much a volunteer here in Madison. So the '70s and '80s witness incredible growth, especially neuroimaging. CAT scans came. This is the first EMI scanner and the first pictured from 1971. I took this picture in 2005 in England in the Science Museum. Then MRI came. We got this unparalleled detail of looking at the nervous system. When I once talked to my father, who started practicing in 1950, they didn't have much at their disposal. It was basically clinical exam, you could do plain x-rays, do spinal tap, and some simple blood tests. This was beginning of electroencephalography, but mostly physicians depended on clinical examination. Now we have these fantastic tools. We are beginning to understand the molecular biology of many conditions. When I started as a neurologist 25 years ago, we had no understanding about Duchenne dystrophy, named after this great French neurologist. Now we understand the molecular biology of this. We hope that some new treatments will be developed soon. So now we are almost at the end of this lecture. Now Dr. Sutula holds this special percussion hammer. He was appointed chair in 1995 and has served for the last 17 years. He's an internationally recognized epileptologist. He's one of these unique persons that still can combine clinical work with basic sciences work. And he has his own lab which is very well funded. That's very difficult to do now. So, we continue to grow. We continue to train neurologists. Our graduates practice on all continents in different countries. Many of them are chairman of departments. Dr. Forster himself trained 16 chairpersons of different departments. Quite an astonishing accomplishment. So, this is one of the last slides just to show you in our department, in our university, we always look to the future but we respect the past. This is a keystone building, for those who don't know. This is the oldest building on the campus. As I understand, it was built in 1836. Eventually, it was purchased by WARF, by Wisconsin Alumni Research Foundation. That's where the Max Kade Institute for German-American Studies and also now the Institute for Midwestern Cultural Studies is located. So, the most important legacy that we have is not so much the accomplishments in terms of number of papers and number of publications but rather the people we train over the many, many years who will train some other outstanding neurologists, and this is the most important legacy that probably I would like to keep in my memory. So, I will finish with this slide. As I said, my father was a neurologist. He's now 91. And my aunt is a neurologist. I probably have something in my genes to be a neurologist. This is my daughter Gabriella, who is a geneticist, graduated recently from UW. Maybe she'll be a neurologist. So, that's the end of my presentation. Thank you very much.
APPLAUSE
Search University Place Episodes
Related Stories from PBS Wisconsin's Blog

Donate to sign up. Activate and sign in to Passport. It's that easy to help PBS Wisconsin serve your community through media that educates, inspires, and entertains.
Make your membership gift today
Only for new users: Activate Passport using your code or email address
Already a member?
Look up my account
Need some help? Go to FAQ or visit PBS Passport Help
Need help accessing PBS Wisconsin anywhere?

Online Access | Platform & Device Access | Cable or Satellite Access | Over-The-Air Access
Visit Access Guide
Need help accessing PBS Wisconsin anywhere?

Visit Our
Live TV Access Guide
Online AccessPlatform & Device Access
Cable or Satellite Access
Over-The-Air Access
Visit Access Guide
 Passport
Passport
















Follow Us