The Canine Influenza Outbreak
06/02/15 | 47m 14s | Rating: TV-G
Keith Poulsen, Diagnostic Case and Outreach Coordinator, and Kathy Toohey-Kurth, Virology Section Chief, at the Wisconsin Veterinary Diagnostic Laboratory, explore a new strain of canine influenza virus affecting dogs across Illinois, Wisconsin, Indiana and Ohio. The strain, H3N2, is believed to be similar to the Asian strain of H3N2 which may also affect cats.
Copy and Paste the Following Code to Embed this Video:
The Canine Influenza Outbreak
Welcome, everyone, to Wednesday Nite at the Lab. I'm Tom Zinnen. I work here at the UW Madison Biotechnology Center. I also work for UW Extension Cooperative Extension, and on behalf of those folks and our other co-organizers, UW Biotech Center, the Wisconsin Public Television, Wisconsin Alumni Association, thanks again for coming to Wednesday Nite at the Lab. We do this every Wednesday night, 50 times a year. Tonight, it's my pleasure to get to introduce to you two folks. The first one is Keith Poulsen. He grew up here, or was born here in Madison, grew up in Waunakee, got his bachelor's degree in biochem here, got a doctorate of veterinary medicine here at UW Madison. Did an internship at North Carolina State, then came back here for a PhD in the Food Research Institute. Then was on faculty at Oregon State University in Corvallis for a while, then came here, came back to Madison to join the Wisconsin Veterinary Diagnostic Lab. The kickoff speaker will be Dr. Kathy Kurth. She also was born in Madison. She graduate from Sun Prairie High School, got a bacteriology degree here at UW Madison, bachelor's and master's. But she got her PhD up in Minnesota. (audience laughing) And she like Minnesota, or M State so much that she went to NIH's Rocky Mountain Lab in Montana and then went on to Plum Island, which is in New York, is that correct? And has a BSL-4 facility. So if you're ever feeling like you need to work in a BSL-4 facility, Plum Island is your place. In 2001, she came back to Madison to work at the Wisconsin Veterinary Diagnostic Lab. Tonight, Keith and Kathy are going to talk with us about the canine influenza outbreak here in Wisconsin. Kathy's going to lead off. Please join me in welcoming Kathy Kurth to Wednesday Nite at the Lab. (audience applauding) So, I'm head of the virology section at the Wisconsin Vet Diagnostic Lab, and I'm going to give a little background of influenza virus in order to kind of prepare for more practical discussion that Dr. Poulsen will lead. So the overview, I'll talk about influenza characteristics, about the new and the old virus, canine viruses I'm talking about, and then the diagnostic assays that we use, and then Keith will take over and talk about the distribution of the virus and answer questions, or at least talk about the most frequently asked questions. The influenza virus genome is a segmented genome, and it's a negative stranded virus. The three parts of the three segments that I'll be talking about mostly today are the hemagglutinin, the neuraminidase, and the matrix. The genes that encode those proteins. So that's what I will be focusing on. This diagram here is showing a cutaway version of the virus particle, and then you can see the eight segments here in the interior part. All right, so the first protein that I'll talk about is the hemagglutinin. There are 16 hemagglutinin subtypes. And all of the work that I'm talking about here is referring to influenza A, type A. So this is the type that infects both humans and animals and also birds. For the influenza A, type A, we have 16 subtypes for hemagglutinin. All of these H types occur in wild birds. There are two additional hemagglutinin types that are found only in bats. So hemagglutinin is a major immunogenic protein on the surface of the viral particle. And in this diagram over here, you see that the hemagglutinin is represented by these blue globules on the surface. That's a little legend on there. The purpose of the hemagglutinin is to allow the virus to bind to the receptor on the whole cell. So the receptor that it uses are the sialic acid residues on the surface of the cell. The other important thing to know about hemagglutinin is that it's very important to be cleaved. It's actually two dimer, and that dimer has to be cleaved before it's active. The second protein that I'll be talking about is the neuraminidase protein, and in this diagram here that I'm using it's this rose colored globules that's represented here. There are nine subtypes for type A influenza, nine neuraminidase types. And all nine of those subtypes occur in wild birds. There are two additional types that have recently been found that occur only in bats. The second, it's the second major surface antigen. We do form antibodies to the neuraminidase. It serves an important role in virus replication, in release of the virus. Once the viral progeny are made within the interior of the host cell, they have to be released, and what the purpose of this, it's actually an enzyme, it cleaves the terminal sialic acid so that viral particles can be released out of the host cell. So it allows the virus to detach and exit. And so it facilitates replication by freeing the viruses. All right, now, you would think that if something's an H3 and an N2 type, that all the H3 and N2s would be similar, but that's a point that I will spend a little bit of time on tonight because they can be very, very different. And that will depend upon the lineage and the geographic region. Two viruses of the same H type can be very different, and also the same N type can be very different. So the diversity will depend upon the species that it came from, the species lineage. Like the avian lineage, all of the viruses or the segments of the virus came, are avian derived. It'll be very different than one that is totally human. The geography will also play an important part. The viruses that evolve and circulate in Asia are very different than the ones that could circulate here in North America. This diagram over here is kind of showing how you know you can have these different H types, we've had H3, H7 found in horse. H10, there influenza A, can be found in sea mammals. H4, H7, H13 have also been found in sea mammals. The hemagglutinin types H1, H2, and H3 have been found in pigs, and all of the H types and N types are found in ducks, as I've mentioned earlier. For H5 that can be found in birds, it's been found in large cats, and then... Okay this looks like raptors there, and then for H5, H7, and H9, that can be found in commercial chickens. So then in humans, H1 through H3 and occasionally H5 and H7 can be found. This diagram is a little bit dated because now we know that there is a new canine virus that was actually found in 2005, the H3N8, that was found by the Cornell group and has been circulating primarily on the eastern coast since 2006. And most recently, then, we've discovered an H3N2 canine virus. How do we get so many different mixes? And influenza has got some characteristics that are really important and help to explain the rapid evolution of that virus. There are mutations in the genome that can lead to subtle antigenic changes. So you can just have one amino acid change, and then, you know, the antibodies in the human aren't going to recognize it as well. So that can a real subtle change that can occur over a few years. So those are just like point mutations in the nucleotides that give rise to a residue change in the amino acid of hemagglutinin or neuraminidase. It's an RNA virus. There's a high mutation rate in general with RNA viruses because the polymerase that's used by the, well, that is encoded by the virus does not have proofreading, and so it naturally incurs a lot of mutations. So this is just kind of stepping through that. So if you have a mutation, a point mutation in the nucleotide, there will be, it can give rise to an amino acid change, and that can alter the epitope on the surface of the virus so that the body, the human, no longer recognizes it. The immune system no longer recognizes it. If you get these small accumulations of point mutations, it will lead to outbreaks, and then large accumulations can lead to epidemics. Now, where we really get into trouble is with antigenic shift. And here, this is, this can occur, well, you can get very, very rapid shifts, changes in the virus with antigenic shift. And it's due primarily to the segmented virus here. These segments, you can have more than one segment. Usually you only have one segment of each set of eight infecting or becoming part of the viral particle. But sometimes you can have more than one of a hemagglutinin infecting the particle. You can get more than one in there or you can have, when it packages, it can reassort from, whoops, I pressed too hard. It can reassort, like it can form, it can take parts of segments from three different viruses. So here we have a reassortment. One of the genes is from a duck, one from a wild bird, and then here one from a chicken. So you'll get a combination here of viral particle that is derived from three different lineages. I just want to make sure I talked about everything. Yep. All right, so, how did we come up, so that's just some background because I'm going to be talking about hemagglutinin and neuraminidase quite a bit, and just kind of wanted to give, kind of lay that background a little bit. What happened here with the canine virus, the new one, we started noticing in March there were some sick animals and a lot of veterinary clinics send their samples to private labs. And so the private labs were noticing that these, or vaccine companies were getting reports of a breakthrough of the vaccine. The vaccine is directed to H3N8, the original canine virus. And they were getting complaints that there were animals getting sick, and it seemed to be a vaccine breakthrough. And so that company started sending samples to Cornell because Cornell had the reputation for being the influence of the canine influenza diagnostic lab. So about mid-March, they were receiving a lot of samples at Cornell, and these were testing positive to a broadly reactive matrix assay. So I should back up a little bit. It's really important when you're testing, when you're just doing a screening assay for influenza that you use a broadly reactive matrix assay. The matrix is a very conserved protein, and when we designed our matrix, we aligned sequences from all the species that we could, human, animal, marine, mammals, in order to try and find the most conserved region. And often, these assays then are a mixture of primers of assays in order to make sure that we can catch all the different lineages. It was really key that Cornell was also using a broadly reactive matrix assay. And the one that they're using was the one they had a plan deviation to use this. They had permission to use this. It was the National Animal Health Laboratory Network broadly reactive matrix. So as you can imagine for all of our surveillance that we do for the USDA, for avian influenza, for swine influenza, we have to have a broadly reactive one to pick up all the different species. They were using that one, and it worked well. It called these positive. But they were unable to type it serologically or by PCR, so we also had some, and I'll go over those assays in a little bit, we have some rapid diagnostics we can do to tell us what type it is, whether it's an H, what H type and which N type it is. And those were not working on this particle, on these viruses. On April 6th, we had our first positive case, and this was a case that came through the School of Veterinary Medicine clinical section, the medicine section, and the dog was showing respiratory disease, so they ordered or respiratory panel. And part of that panel is influenza A, and so we did, we were able to detect a matrix positive in this animal. And so that was on April 6th, and a few days later, Dr. Glaser at Cornell, who runs the diagnostic section there, is a friend. We are on a lot of national committees together, and so I called her to ask whether they had started typing, as far as if they knew whether it was the same or not. And they had started working with it. And we kind of, well, we started a collaboration. And on April 10th, we used a neuraminidase assay that we had developed several years ago that, again like the matrix, we planned it to cover all species as well as we could. And it did type as an N2 with our assay. And then the same day, Cornell got some sequence data on the matrix gene and also the hemagglutinin gene that showed that it was not the H3N8 that had been circulating for a decade. We knew we had a new beast and that it was a, sorry, that it was an N2, and the sequence of the hemagglutinin showed that it was an H3, but it was very different than the H3 of the H3N8, the first canine virus. And then April 16th we got the complete genome, and that was done in collaboration with Dr. Mia Torchetti's group at the National Vet Services Lab in Ames, Iowa. They had one of the beauties, well, one of the newest techniques that is available to us now is next generation sequencing, and that's what Dr. Torchetti used in order to get that genome so quickly. This new virus, H3N2, it's 99% related to an Asian avian derived H3N2. So, it's most closely related to one that's recently been circulating in Korea. The first, it was first noticed in China, in Guangdong province in 2006 in pet dogs. And the viruses characterize as avian in origin because all eight segments are derived from an avian lineage. And the virus, it's very close. Ours is 99% related. So we don't think it underwent any change here. It was just like an introduction of that virus from Korea directly here. It's been circulating widely, well, in China and in South Korea, since it's initial discovery. In terms of relatedness to the H3N8, the hemagglutinin has about 71% homology. So the nucleotides, when you line them up, about 71% are exact. The neuraminidase only shows about 50% homology. Oops. That one I didn't quite... So, how do we test for the presence of a virus? I just want to go over our diagnostic assays a little bit because that's what we do at our lab. Basically, you can look for the virus itself, or the nucleic acid for the virus. Either the proteins on the surface of the virus or the nucleic acid within the virus, or you can look on the left-hand side, you can look for the antibody response. So it's the person or animal's response to the virus. One of the tests, the clues at Cornell was that they had an antibody detection system. It's called hemagglutination inhibition, and it wasn't working on this virus. So the virus was so different that it wasn't, you couldn't do this agglutination assay, this agglutination inhibition assay. We are hoping to develop a serological assay for antibody detection in order to answer some kind of questions that I'll get to a little bit later hopefully later this summer. In terms of looking for the virus itself, we have spent a lot of time in the past decade developing real-time PCR assays because they're very rapid and they work in a high throughput system, and in our lab we might be running like 500 in a day, different assays for different species. So we try and get everything on the same system so we can do it very efficiently. So, with real-time PCR, that reason it's become so popular, and it's really a workhorse now in veterinary diagnostics and also in human diagnostics, is because you can, whoops, sorry, sorry, sorry, because you can watch the progress of the reaction as it works through the cycling parameters. As the name implies, real-time, you can watch it in real-time. I don't know if very many of you have ever run a gel, have done PCR the old fashioned way where you had to take the product and run it on an electrophoresis gel, you don't have to do that with real-time PCR. You don't have to run any messy gels or anything. It's all closed tubes. So you set up your reaction in that one tube. You shut it, and then you're done. You put it into the instrument, and that really cuts down on contamination. So that's one of the things we worry about in a diagnostic lab. We want to make sure that we don't have any contamination that we're introducing into the sample. We like that for that closed tube. It helps prevent contamination. It's real-time so we can watch what's going on. It's also very rapid. We can get an assay done in a couple hours, and so we'll know the result. The way that we read out these assays, so you can see the multicolored lines there, the background fluorescence. I'm a little bit scared. There. -
Man
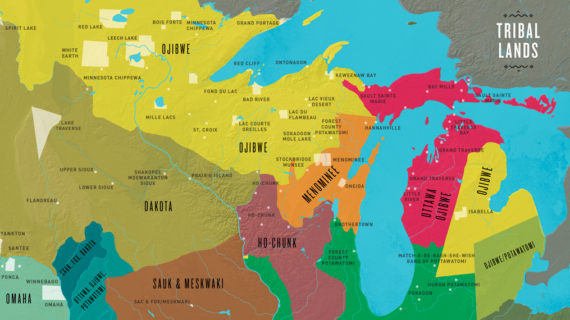
Can you say what a PCR is. Oh, I'm sorry. Polymerase chain reaction. Polymerase chain reaction is a way to multiply very small amounts of targets, like say you have a sample from someone that you know is sick but they don't have very much of the virus present, so you can take, if they just have very small amount of that virus present in that sample, like say it's a nasal sample, you can take that sample and put it in an instrument, like a PCR machine, and it's basically like a photocopy machine. You can take one page and photocopy it, and you'll get, actually if you start with one target organism, you can end up with 10 million at the end of three cycles. So, basically, PCR allows you to replicate that target every cycle. So a cycle basically is allowing the strands of nucleic acid to separate. The first part of the cycle is high temperature. So the strands separate, and then you have little pieces of DNA that find its match, matching target. And then the second part of the cycle is to allow annealing and extension so that you'll get, from that separation you'll get two copies made, and then those two copies are heated and, in the next cycle, they each are replicated twice. And so by twos you increase. You go from one copy to 10 to the million in like 30 to 35 cycles. We typically run about 40 cycles here for our real-time PCR assays. If an assay is very efficient, we should be able to replicate it, all of the copies in that test tube. So we do everything in a very, I'm going to show you in this next... We do everything in these small, little microfuge tubes. So 96 of those little tubes will fit into a well, plate like about this size. So they're very small tubes. And if the assay is designed correctly, it will increase double every cycle. I'm just going back to this one. When we do real-time PCR assay, what we want to look for, the reason why we can look at the, find the results within the time that the cycling is occurring is because of the production of fluorescence. We have background fluorescence here that the instrument deletes. And then, if we have a positive, sorry, I'm just a little bit too sensitive here. I'm going to have to point. If it rises above the threshold, the threshold is a line that's drawn by the instrument to separate the background fluorescence from a true positive. So you'll see that... Try again here. So you'll see this amplification curve that is rising above the green line, and so that's indication of a positive sample, and it's crossing the threshold very early. We do about 40 cycles. So this is crossing at 21 cycles. After 21 cycles where everything is doubled, it crosses the threshold. That means there's a lot of virus present. If it crosses late, like here at the end, sorry, the second one where it says positive, there's not very much virus present. We can just tell by the amount of fluorescence then, and then these read-outs that we get, we get a list of values that says either negative or the CT is 21 or the CT is 39. So we can know from that report then whether we have a positive or not. For our neuraminidase typing assay, we do a multiplex assay. So it's also a real-time PCR assay, but this time we have more than one in there. We have the matrix in there, and then our N2 assay and N8 assay. In this one reaction, we can figure out whether something's influenza A-positive and then also which type it is. Is it the old canine influenza, or is it the new canine influenza? Just to kind of summarize what we found in Wisconsin so far, there's been one positive at the School of Veterinary Medicine. And this dog had been Chicago the previous week before it got sick. And there were two cats and one dog at the house where it lived, and those animals did become sick, but by the time we tested them for the new virus, it was beyond the time when we could detect it. So that was not confirmed. And we've also had one positive submitted by Marshfield Clinic, so I don't know exactly where in Wisconsin that is. I know where Marshfield is, but they get samples from all over. And then there's a private firm. Like I said earlier, a lot of the veterinary clinics will send their samples to private companies. They went back and looked at all their samples. They actually had an assay that was missing the new virus. And so all the things that they tested in March they had to go back and retest, and then they informed the clinics. And so there were three other positives in the Milwaukee area. One of the things that helped us a lot with this is to get the complete genome testing, and this is something, we used an older technology called Sanger sequencing, but the newer technology, next generation sequencing, allows us to get the whole sequence very, very quickly. And that's what NVSL use. We were mentioning earlier about how PCR changed everything, well, I think this next generation sequencing is going to be the PCR of the future because I think that that's all we're going to be doing probably in about 10 years. We save questions for later. Okay. Do you have your own? - Yep. - Okay. So, I think Dr. Kurth had the hard part talking about the basic science and, really, what the nuts and bolts of everything that went through to actually find the virus and type it as new. I have the easy part, to come by and talk about, really, the majority of what I've done with this as part of the WVDL team is to talk on the phone. There's a couple people at the lab that really like to talk on the phone. I'm one of them. Dave Krueger is the other one in virology, and I think we spend a good part of our day actually speaking on the phone and talking to not only veterinarians that are our clients, we have lots of dog owners that call in, and then with the media as well because the university release, press releases talking about what's going on, so then we moved it into the general media. As part of this, as it came through, Dr. Kurth talked about working with Cornell and IDEXX is a private lab and then Merial, which is another pharmaceutical company that does quite a bit of veterinary biologics, specific biologics, and they actually are one of the makers of the older strain of the virus H3N8. I was sitting at my desk, and after going through all of the different phone calls and I got another one that said, well this is Jonathan calling from Princeton, he has some questions. And I thought it'd be some more influenza questions, and he said, and this is what really made my day, he said "Hi, I'm John, "I'd really like to talk to you about your data. "I'm an epidemiologist, "and I'd really like to organize the data "and really look at it." I thought, "Oh, thank, thank God." It's really helpful to be able to take multiple different groups, whether it's at different institutions or private industry, and then collate that data together. And really, that started a conversation to take what we're finding at the Wisconsin Veterinary Diagnostic Lab and really collate it with all of the other labs, including Davis and IDEXX and Cornell. So that's what really came out and brought apart this national canine influenza task force. And really, what we're charged to do is really disease ecology. How is this disease different? What's the attack rate? Are dogs really, do they have more severe disease, or is it just because it's a new disease? What are we likely to see in the future? What have we seen in the past? So that's really how Princeton really works into this group because there isn't a veterinary school at Princeton that's why I was not expecting someone to call up and ask to really delve into the data from there. Another big component of this, which isn't on this slide, is the University of Wisconsin, the School of Veterinary Medicine shelter medicine program, which is relatively new, and it's headed off by Dr. Sandra Newbury. And she's, along with the Kurth lab in virology, is really looking at an analyzing a lot of the positive samples in Chicago, which are coming out of animal shelters. So, from there, this is one of, Cornell has a GIS, or geographical information systems, department. It would be great to have something like this to be able to tell you if it's in Dane County or Oconto or Green County. But this is what they would do. They took all of the positive tests, and this is nowhere near what is probably actually going on. This is only what's actually been tested. If you think about everything else, you've go to look at this as an estimate. What they did is they took all the positive cases and they put them into a map. And this is accurate as of May 16th. I'm expecting them to have one accurate as of June 16th or maybe June 10th. I know they're close because we just gave them a whole slew of data. Because you can see here, Texas is still zero out of six. So we know that there's more positive out there, and you're going to see how this map changes, and anyone can search this. If you search "Canine influenza Cornell," you'll come up with this map. The other thing that's going to be a little bit different, how many people in here that go to the doctor every time they get sick? Not everyone, right? And then you also have that when you go to the doctor, do they always get tested for disease X, Y, or Z? Not all the time, right? And then even of those people that are tested, the test isn't always positive because you might be too far or away from the onset of clinical signs. So, that's what the beginning part of this disease is, and I think as we get more and more data in, we'll be able to really hone in on what is really actually going on. And when you look at even CDC's page for different human diseases, those are typically usually estimates, okay? The big thing that I really want to go through now is, well, what are all the frequently asked questions that I got? These are the top five or six questions that I think either myself and Dave Krueger are asked every single day.
And here's the first one
what do I do with my dog? How many people in here have dogs? How many people were worried about their dogs with influenza, right? A pretty good proportion of people because it was in the mass media, whether it was internet, TV, or radio, or even press, so in the Wisconsin State Journal. And really, what I was interested in, and some of it kind of got a little bit different every time I did interviews or talked to dog owners, is that if you think about influenza, what do you do when you're sick or when your kids are sick? You usually keep them at home or you stay away from sick people that you see in public places like airports. And this is one of the things that are near and dear to my heart. I have two toddlers at home, right? And you're not allowed to bring sick toddlers to daycare, right? And it's very just kind of common sense. But when you remember about common sense and large groups of people, common sense usually isn't right on the top of their list, right, okay? That was kind of one of my jokes that actually made it into one of the interviews, and I said that to my wife. I said, "Hey, my joke finally made it in." and my wife, who's a small animal veterinarian in Lodi said, "You're still not funny, husband, just keep working." (audience laughing) But I still think it kind of makes me chuckle. Keeping my dog at home. How do you know your dog is sick? Things that we look for because canine influenza is really only part of canine cough syndrome. Now, I'm probably the last person to talk about canine diseases because I'm a dairy veterinarian. If it wasn't black or white with black spots, I really didn't know much about it. But now, as a very different, as my career path has moved on, I really have spent the majority talking about dog and avian diseases in the last few weeks. So, canine cough syndrome. So, there's a bunch of different things that cause, and I should say things, we're talking about pathogens. So there's bacteria and viruses that, that may cause your dog to cough. Any of you that have had a dog at a dog park or a dog at maybe boarding or even at your veterinarian overnight may have come back with something bordetella. So, kennel cough. Kennel cough is something that you probably heard of or you might see warnings of at the dog park. That's probably the most common reason why we see dogs coughing. My dog's had kennel cough because I brought him to school when I was a veterinary student. Bordetella is a bacteria that can do it. There's other viruses that can do it. Different types of influenza that may or may not be causing your dog to cough. Other things that we think about with coughing. What else happens with coughing? You have nasal discharge, right? That's not clear. You can't see through it. That's when you know there might be something going on. Or you might have ocular discharge. Your eyes run because all those ducts are all connected. Dogs are no different than people. They're just longer ducts with longer noses, right? Nasal discharge, eye discharge, cough. What else happens when you have the flu? You have a fever. What does a dog look like when they have a fever? Same as we are. Kind of lethargic, more than usual. You know, my dog doesn't really do much. She's a little bit older, but they don't want to go out and play with the ball, or they might not want to eat. You get those body aches, and you just don't want to eat. The same as you when you're sick. So, you might not have a fever, they might not have an appetite, and they'd be lethargic. So those are the things you'd really look at for whether or not you should take your dog to the dog park or to other dog events, like puppy up in Dane County, which happened about six weeks ago. Those are the big questions that we had coming on is that, what do you know? I know that working with Sandy Sawchuk, who is part of the community practices at the university, she really said, you know, "Maybe this is the time where you have your dog on a leash." When we're not quite sure what's going on, this is the time that you have your dog on a leash until the outbreak is kind of gone over on the tail end. What about can I catch CIV from my dog, right? Everyone gets pretty worried about influenza. When you had the H1N5, all the different Hs and Ns, you had swine flu or now we have equine influenza or avian influenza, there's lots of different types of influenza that we hear... Whether you're reading the internet or you see it on the TV news. The one thing we can say about canine influenza is that we haven't seen any reported human disease from that. Could it happen in the future? Maybe, but we haven't seen it yet. We think it's a very low chance. Although, there are other H3N2s that have been reported to affect people in Asia, but those are very different strains. You remember what Dr. Kurth talked to you about several slides ago is that they're all very different depending on what species that they're in, right? But remember the influenza is a very dynamic pathogen, so that's why we watch it very closely. So, no, the answer to that to me would be no, very unlikely. Do I vaccinate my dog? How many dog owners in here had their dog vaccinated for flu? This is all my wife did for several weeks. When this outbreak came across in April 6th, so the second or third week in April, her appointment catalog or her appointment schedule got book right away, and they're almost all influenza vaccines. And then people started to get really upset because the supply of influenza vaccine did not meet the demand. Now, that doesn't really make sense, right? You can always got to Walgreens and get an influenza vaccine, right? Or CVS or your doctor. It's not quite the same economy of scale for veterinary species. So, when we're talking about the vaccine that's commercially available at this point, it's very species directed. So, it's very species directed to the H3N8, and that's the circulating strain in this area and in the United States since about 2004. Now, it's not a core vaccine. So, what a core vaccine would be animals that come through every year or every three years, depending on how old they are, they get a core set of vaccines that's recommended by the AVMA. Very similar to a core set of vaccines that a toddler gets from the Pediatrics Association. My kids are getting vaccinated in a couple months, so that's on top of my list. So, it's not a core vaccine. So not everyone uses it, so not every veterinarian has huge stocks of it because it goes bad, right? It goes past the expiration date. That was one big thing that we talked about is that who needs to be vaccinated and what happens when we don't have vaccine is a lot of people get really frustrated. When I say who needs to be vaccinated, the vaccine, even though it's directed against an older strain, we still held out hope that it had some cross protection, and depending on what virologist you talked to, virologist or veterinarian, they had varying levels of cross-protection, but we were all pretty much in agreement that it would be low, okay? But we always say do no harm. So those dogs that are of high risk for a potentially new strain, so whether it's a dog that has to go to doggie daycare, at least a couple days a week, or it has to go to be boarded when you go to Europe for two weeks over the summer, those are the dogs that will be at a higher risk because they're in a dense population of dogs. So those are the dogs that we're recommending to be higher on the priority list for vaccine. So, what about a new vaccine? So, as part of vaccine isolation, whether it was Cornell or Wisconsin, we all collaborate with the pharmaceutical companies and share isolates to hopefully have a vaccine available, whether it would be multiple companies, hopefully in the near future. I don't know how long it's going to take the FDA to approve these vaccines. I'm hoping it'd be six months to a year, but I know that what they've told us is that they're fast-tracking it. Now, whether or not that's going to be a separate vaccine or it's going to be a multivalent vaccine, it's unknown to me at this time, but it would be directed specifically at the clinical isolates that we've gotten. So, vaccinating my dog. I would say talk to your veterinarian. That's going to be your best bet. It's not going to be, especially in the course of an outbreak, your dog isn't going to be protected with any vaccine after one dose anyway. It's a two-dose booster, and it's going to take several weeks to build up active immunity to prevent infection or clinical signs. So there's more to it than just getting a shot. Do I vaccinate my dog? How do I treat my dog that could be infected? So, I have a sick dog at home, and lots of people, and you hear it in the news about overuse of antibiotics, and this is one big thing about, well, if it's a dog with flu, why don't we just give it antibiotics? Remember, antibiotics are directed at bacterial infections, right? So, and this is a viral infection. Now, not to say that dogs infected with viruses don't get antibiotics, or people infected with viruses don't get antibiotics. And the reason why those animals do get antibiotics, or people when you go to the urgent care, is because they're protecting against a secondary bacterial infection. Or if you don't go through and have the diagnostics and it's presumed to be a bacterial infection where it could be a virus, that's where the antibiotics are coming into play. Now, in this case, we recommend supportive care. What do you do for supportive care with the flu, right? You feed the flu and starve a cold, or you starve, I can't remember how that goes. Lots of liquids is really what the common goal in trying to treat and support any fever. So a non-steroidal anti-inflammatories, ice packs, cold compresses. My cousin had a dog that had clinical signs very similar but was not diagnosed, and I told her to watch her very closely, lots of fluids. Dog did okay. But people are worried about because you see the ABC World News is there's dogs dying in Chicago, and they say what about the dogs that are dying? Well, that's a very, very small proportion of dogs. We think it's less than a single digit percentages. We don't really know how many dogs are out there that had died, but we think it's very, very small, 5% or less. Not to say that if that's you're dog, it's still going to affect you pretty severely, but when you think about the population in general, very, very small. The other thing, what do I do if I think my dog is infected? What would you do? What do you do when you think your child is sick or your spouse is sick? Talk to your veterinarian. Not with your spouse. Talk to your veterinarian. We have lots of information on our website. On www.WVDL.wisc.edu, or the School of Veterinary medicine has lots of posts out there. The other thing that I wanted to talk about is Dr. Kurth talked about potentially having cats affected. We haven't seen that other than the anecdotal reports. We haven't seen a test positive cat. Not to say that they're not out there because that's a big difference if you're thinking about or I know they're thinking about having an avian influenza talk in July. There's two influenzas going on at the same time here, right? But we know lots more about avian influenza because all of our results are required to be reported to DATCP and USDA. That's controlled very, very tightly, and all that information, there's an infrastructure to handle that. We don't do that with canine influenza because it's not a reportable disease. We're doing the best we can with voluntary admission of results from the different labs. I do, I actually went out and tested those cats that we were talking about. I went out with Dr. Chun, who's the associate dean of the teaching hospital, and I have to say it was hard. After we chased the cats down. (audience laughing) Anyone who has a cat, unless they're a weird yellow tabby like what we have at home, we chased those cats for almost an hour. And by the time we got these, I guess overweight is the best way to say it, they're happy cats, by the time we actually chased them and cornered them, they were doing the same thing I was, was holding the sample trying to catch my breath. They did have an increased respiratory effort, but, again, those cats were noted to have clinical signs two to three weeks before when we actually got to test them. So I would still watch my cats too, if you had other cats and you had sick dogs on the farm, at home as well. So, those are the major frequently asked questions that we get every day, whether it's at the School of Veterinary Medicine or at WVDL. With that, what's going to happen in the future? There's a lot of things, a lot of data that's got to be sifted through, and hopefully with the canine task force with the multiple different institutions in the United States and the private labs and pharmaceutical companies, we'll know more about the disease ecology or the pathophysiology of how this virus came about, what we can expect from new infections. I know that another thing that we look at is new infections. We seem to see more severe disease, but you've got to remember, this is a naive population. So this is a population of dogs in Chicago, and Chicago is very densely populated, right? So it's a naive population that's seeing a new virus. We are going to see more clinical signs regardless of whether or not the virus is stronger or more potent or more pathogenic than the previous one just because we have a population that's never seen it before. So, hopefully we get most of that data back within the next months to a year, and hopefully we're working on publishing that so it's out into the peer reviewed literature. With that, we have a little bit of overlap, but I really, for Dr. Kurth and myself, I thank you for your attention, and I know after we're done taping, we'd love to take questions. (audience applauding)
Search University Place Episodes
Related Stories from PBS Wisconsin's Blog

Donate to sign up. Activate and sign in to Passport. It's that easy to help PBS Wisconsin serve your community through media that educates, inspires, and entertains.
Make your membership gift today
Only for new users: Activate Passport using your code or email address
Already a member?
Look up my account
Need some help? Go to FAQ or visit PBS Passport Help
Need help accessing PBS Wisconsin anywhere?

Online Access | Platform & Device Access | Cable or Satellite Access | Over-The-Air Access
Visit Access Guide
Need help accessing PBS Wisconsin anywhere?

Visit Our
Live TV Access Guide
Online AccessPlatform & Device Access
Cable or Satellite Access
Over-The-Air Access
Visit Access Guide
 Passport
Passport
















Follow Us