Impacts of Fighting COVID-19 on Frontline Health Workers
By Marisa Wojcik | Here & Now
September 24, 2021 • West Central Region
Reporter Marisa Wojcik investigates an intensive care unit at Marshfield Clinic as COVID-19 cases continue to rise in Wisconsin, exploring severe stains on ICU space in hospitals and the perspectives of the frontline health workers who continue to fight the pandemic.
“The pandemic was looking like it was essentially over two months ago. We had zero to two, maybe three patients in the hospital,” said Dr. William Melms, chief medical officer for the Marshfield Clinic Health System.
“Today, we watched the state of Wisconsin, the number of new patients continues to rise and the new patients per day are the kind of leading indicator of what we can expect. So we have grave concerns yet that we’re not near the end of this surge,” he added.
During rounds in a covid ICU, doctors, nurses and residents are busy discussing each patient’s progress and treatment plan. Patients are there for weeks, usually in a medically-induced coma as machines work to save their lives.
“Everyone is seeing stuff in the news, and they don’t believe it until it’s happening to them,” said Ryan Letsch, a covid ICU nurse.
“Or they do know what’s happening and that makes them even more scared,” he added.

Marshfield Clinic ICU staff prepare their personal protective equipment as they work in a ward treating COVID-19 patients. (PBS Wisconsin)
Letsch specializes in administering a respiratory treatment called ECMO.
“What ECMO does is we’re allowed to have the lungs do basically nothing as we oxygenate through the machine and keep the patient’s brain and heart and kidneys all healthy with oxygen,” he explained.
It can be the last tool health workers have to save a patient’s life. But ECMO resources are limited and in high demand across the country as the Delta surge continues to worsen.
“The patients are sicker this time,” said Vicky Varsho, a chief nursing officer at Marshfield Clinic. “We see that they’re deteriorating quicker as well and being sicker requires more resources.

A regional chief nursing officer at the Marshfield Clinic, Vicky Varsho notes widespread demand for hospital resources as the pandemic has worsened again. (PBS Wisconsin)
Varsho said Delta is inundating health systems everywhere.
“We’re getting calls from Canada. We’re getting calls from the east, from the west,” she said. “We’re getting calls from people we’ve never received their patients from before because they are so strapped for beds and resources as well.”
Letsch sees the ruin this disease leaves every day, comparing it to a hurricane, leaving destruction in its wake.
“There’s definitely a different feeling when we’re putting a breathing tube in these COVID patients just because so often we’re not able to hear from them again. And knowing that, going into the breathing tube is very, very difficult,” said Letsch.
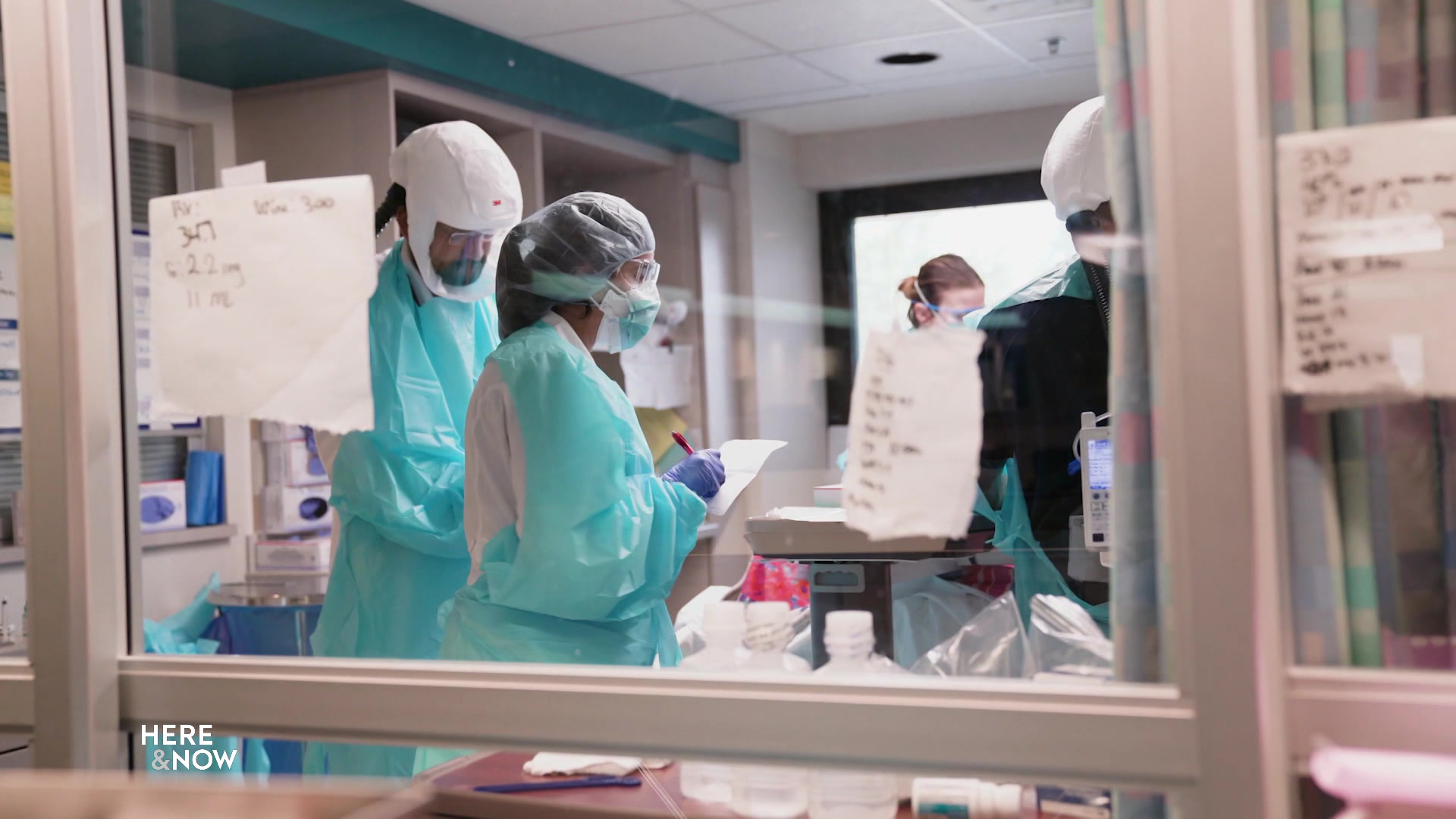
Clinical care at a Marshfield Clinic ICU ward attend to a patient fighting COVID-19. (PBS Wisconsin)
Their stories endure and so does the trauma.
“Having to convey or do FaceTime with these patients and their family, we’re really — we’re the middleman, having to say hello to their son who’s going to college for the first time or people are getting married,” Letsch shared. “Watching them have to see it through a tiny camera on their phone while they’re intubated is very tough.”
Staffing shortages were a problem before 2020, and the pandemic has made it worse as many health care workers leave the profession.

Marshfield Clinic ICU nurse Ryan Letsch relies on limit ECMO resources to help save the lives of COVID-19 patients. (PBS Wisconsin)
“Worsening burnout turns into a vicious cycle because they leave health care, another new person replaces them and the issue isn’t fixed so they get that burnout all over again,” said Letsch.
The emotional toll is greater now, as the issue of the pandemic rolls on and the patients are not only sicker, they’re younger.
“We have had pediatric cases. The youngest patient we had was four months old,” said Melms. “The demographic of the patients we admit in our facilities are certainly younger than they were last year. Absolutely the case. Absolutely the concern.”

As chief medical officer of the Marshfield Clinic Health System, Dr. William Melms is concerned about how much the Delta surge in the COVID-19 pandemic might grow. (PBS Wisconsin)
Health officials are hoping more people will choose to get vaccinated against COVID-19 in the wake of this latest surge.
“Even some family members who were very against the vaccine, it’s a lot different when they’re crying over their spouse,” said Letsch. “Every single one of them have gotten the vaccine that day of admission or the very next day.”
“The frustrating aspect of this pandemic is that we could be preventing so much of this and we’re not,” Melms said.
 Passport
Passport









Follow Us