A Sprint Between Variants and Vaccinations Extends Wisconsin's COVID-19 Marathon
Here & Now Extra: As newer and more virulent coronavirus strains gain a foothold in the state, public health researchers hope tracking efforts and vaccinations can keep pace.
By Kristian Knutsen | Here & Now
March 16, 2021
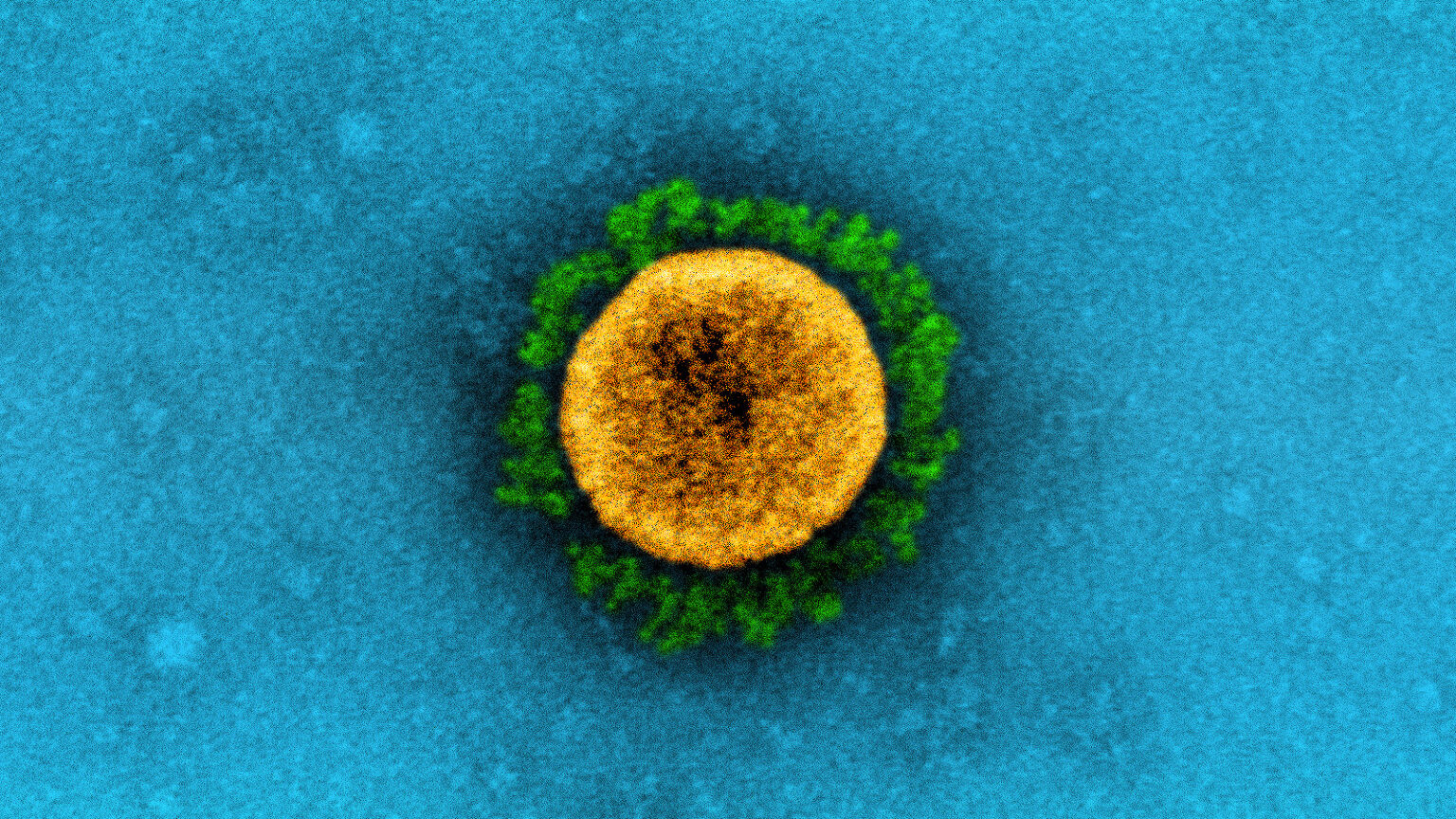
A transmission electron micrograph shows the B.1.1.7 variant of a SARS-CoV-2 virus particle, isolated from a patient sample and cultivated in cell culture. This colorized version shows the spike proteins in green and central virus particle in yellow. (Credit: National Institute of Allergy and Infectious Diseases (CC BY 2.0))
A year after the pandemic started upending daily life in Wisconsin, glimmers of hope are growing into broader optimism. Since the end of 2020, the number of new confirmed COVID-19 cases has plummeted in the state, followed in turn by hospitalizations and deaths. About one in eight Wisconsinites have been vaccinated as of mid-March, and the pace of these deliveries is accelerating. At the same time, though, new and more dangerous variants of the coronavirus are starting to spread, and public health researchers are warning about the risk of reversals.
Several emerging variants of SARS-CoV-2, the virus that causes COVID-19, have been identified so far, and researchers are laboring to identify how their mutations affect how easily they’re transmitted, the effects they have on COVID-19 infections and what they could mean for vaccines. It’s a breakneck scientific race, extending the pattern set since the start of the pandemic, with research and public health efforts sprinting to keep up with the virus.
Nearly 5,000 instances of three different variants — labeled B.1.1.7, B.1.351 and P.1 — had been reported across the United States as of March 11, with at least one variant being identified in nearly every state. These cases are not evenly distributed, but instead have been largely clustered in a handful of states, including Michigan and Minnesota (including a spike in the southwest suburbs of the Twin Cities).
In Wisconsin, 32 variant cases had been identified as of March 11 — 31 were B.1.1.7, also known as the U.K. variant, and one was B.1.351, which is known as the South African variant. This total was out of 7,306 samples tested up to that point, which reflects the limited nature of this surveillance. Relatively few confirmed cases of COVID-19 are genetically tested, and the number of variant cases in the state is thought to be higher than this number.
“Please note that the variant cases identified in this table likely represent a fraction of how many cases of SARS-CoV-2 variants are circulating in Wisconsin,” warns the Wisconsin Department of Health Services in an explanation that accompanies its counts of each variant identified in the state.
The number and breadth of variant COVID-19 cases is quickly becoming a primary concern for public health researchers, as discussed by University of Minnesota epidemiologist Dr. Michael Osterholm in a March 12, 2021 interview on Here & Now. Director of the Center for Infectious Disease Research and Policy, Osterholm served on the COVID-19 advisory board for President Joe Biden’s transition into office, and has been warning about the risks posed by the variants for weeks.
Osterholm likened the situation in mid-March as akin to being in the eye of a hurricane, with the relative calm of low case numbers only a lull in the ongoing storm.
“Everything looks kind of blue skies right now, gentle breezes. But the back wall is coming, and that is this variant, the mutated viruses we see,” he said. “In fact, one in particular, what we call B.1.1.7, which was first found in the United Kingdom, is about 40% to 60% more infectious than the previous viruses we dealt with. It’s clearly causing much more severe disease.”
Osterholm went on to note this variant’s ongoing spread in Europe, and noted that even with the growing (but still relatively limited) number of vaccinations, many Americans remain susceptible to infection. He warned about the potential effects of loosening public health restrictions as variant cases mount.
“Unfortunately, it’s a perfect storm,” he said. “We’re doing everything but turning over our credit cards to this virus. We’re giving it every opportunity to be transmitted.”
Osterholm also discussed the Dr. Doom sobriquet he’s been tagged with in response to his grave warnings about the pandemic, as well as why he has delayed getting his second dose of a COVID-19 vaccine in the interest of preserving more supplies for senior citizens.
How is Wisconsin’s state-level public health apparatus preparing to track the spread of emerging coronavirus variants?
Here & Now extra
Genomic testing of coronavirus samples has been conducted in Wisconsin over the course of the pandemic, and the state has been identifying and tracking emerging variants for months.
The Wisconsin State Laboratory of Hygiene in Madison and several other labs in the state conduct routine whole genome sequencing of coronavirus samples associated with confirmed cases. Their capacities are limited, however, and the number tested are only a small fraction of the total number of cases in the state. As of March 11, the state health department reported 7,306 specimens had been sequenced, a figure that is about 1.3% of the 568,352 confirmed COVID-19 cases reported as of that date. Yet even with that limited sampling, variants are increasingly being detected.
The first instance of B.1.1.7 was identified in Wisconsin on Jan. 12. Echoing the state’s first overall confirmed coronavirus case, the Eau Claire County resident who was infected with the variant had recently returned from international travel. About a month later, a second instance of B.1.1.7 was identified in the state, this time in a sample from a Waukesha County resident. Dozens more instances of this variant were reported in other locations around the state in the ensuing weeks.
Looking ahead, Wisconsin is moving to expand its capacity for coronavirus genomic sequencing through new federal funding. On Feb. 17, the U.S. Department of Health & Human Services announced nearly $200 million to bolster this aspect of testing and research.
According to a Wisconsin Department of Health Services spokesperson, the state hygiene lab is to receive $2,770,142 to expand its capacity to sequence the genomes of SARS-CoV-2, as well as other pathogens. Supporting an expansion in staffing along with equipment and supply costs, the funding will allow the lab to roughly double its weekly genomic sequencing capacity, from about 200-250 specimens up to 400-500. It is budgeted to run up to July 31, 2023, though the new equipment will continue to be used for ongoing genomic sequencing.
This funding was characterized by the Biden administration as a down payment on increasing this aspect of pandemic surveillance — indeed, the American Rescue Plan Act of 2021 includes $1.75 billion for genomic sequencing, an element introduced to the COVID-19 response package by U.S. Sen. Tammy Baldwin, D-Wisconsin. The senator described that funding as the foundation of establishing public health infrastructure to maintain ongoing surveillance of COVID-19 and other pathogens.
The state health department has typically released its data about coronavirus variants on a weekly basis, updating its figures on Thursday afternoons. However, when the first instance of the B.1.351 variant was identified in Wisconsin at the beginning of March, the agency updated its table tracking these cases and promoted the finding via a statement and social media.
Looking ahead, the state is planning to develop a specific data page about variants in its suite of statistics about the coronavirus in Wisconsin, though it doesn’t anticipate adding information about the county of residence or other demographic information about individuals infected with variants, at least at this point in time.
In a March 12 interview on Here & Now, the state health department’s interim Secretary Karen Timberlake urged Wisconsinites to continue following public health guidelines for the pandemic.
“We know these variants are more contagious. They are more transmissible. They spread quickly,” said Timberlake. “That is why between getting everyone vaccinated and continuing to wear masks, watch your distance, wash your hands, all of those strategies together will help us win the race against this virus.”
This race against COVID-19 pits the spread of the new variants against the burgeoning efforts to deliver as many vaccinations to the largest number of people as possible.
A year into the pandemic, nearly one in 10 Wisconsinites have tested positive for the coronavirus. That figure does not include the many people who have been infected by the coronavirus but did not get tested for whatever reason, and determining exactly its scope is yet another focus of COVID-19 research.
The CDC estimates the overall burden of the disease is much higher than what has been reported, and that for the period between February and December 2020, roughly 1 in 4.6 total COVID-19 infections were reported. If that ratio is applied to Wisconsin, it could mean more than 2.6 million of the state’s residents have been infected so far, or roughly 9 out of every 20 people. Of course, such a calculation doesn’t take into account the rate of COVID-19 reinfection, another area of scientific inquiry, including in terms of the emerging variants.
Meanwhile, more than one in eight Wisconsinites have been vaccinated against the coronavirus as of March 16, and more than one in five have received at least one vaccine dose so far. The pace of vaccinations in Wisconsin has been accelerating over the course of 2021, and the state is shortening its distribution schedules.
An expanded vaccine eligibility criteria timeline covering more than two-thirds of Wisconsin adults was moved up to March 22 after having previously been set for March 29. Milwaukee County Executive David Crowley also announced that any resident of 10 zip codes in the city of Milwaukee who is 18 or older would also be able to sign up to get vaccinated starting March 22. Meanwhile, Gov. Tony Evers has said he expects all Wisconsinites who are age 16 and older will be eligible to start getting vaccinated by May 1. These millions of vaccinations require time to be administered, though, and meanwhile the variants continue to spread.
As another spring arrives, public health researchers like Dr. Michael Osterholm remain concerned that this race between variants and vaccinations leaves too much room for another potential surge.
“I know the public doesn’t want to hear this,” Osterholm told Here & Now. “It’s horrible. We’re all at the ends of our rope with regard to this pandemic. But this is, I think, the last big hurdle to get over, at least in terms of the short term. With the vaccine going to be here in May, this surge with this virus lasting 12, 14 weeks — I don’t know — but it’s going to be here for a while and we’ve got to understand that.”
 Passport
Passport









Follow Us